PAs and Social Determinants of Health: 4 Things to Know
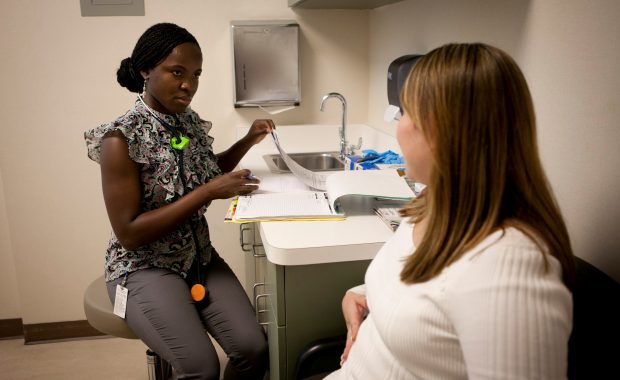
Understanding social determinants of health along with treatment creates a holistic approach that may benefit patients in the long-term. PAs that integrate social determinants of health into patient care see greater satisfaction with care, health outcomes, and patient adherence to medical advice.
July 1, 2020