A Day or Night in the Life of an Emergency Medicine Fellow
Combatting Imposter Syndrome and Training to be Ready for Anything
September 4, 2019
By Stephen Lewia, PA-C

Before starting PA school, I practiced as a Nationally Registered Paramedic for ten years. Needless to say, Emergency Medicine (EM) was my specialty of choice very early in my PA journey. I attended PA school at University of Lynchburg in Virginia. When applying for jobs during my clinical year, I began looking into formal postgraduate training as an alternative to a traditional first job.
I chose a fellowship for several reasons. First, I knew that I learn best in an academic setting. I wanted to learn EM through both hands-on and didactic education. To enable opportunities to acquire the broad knowledge needed to practice Emergency Medicine, EM fellowships commonly include non-EM rotations and training and I personally saw value in the variety of experiences I would gain while in an EM fellowship. Lastly, and to me most importantly, I wanted my professional development to take precedent over productivity. While many have found professional development though non-fellowship opportunities, I decided to seek them in a fellowship.
Choosing the Vituity EM Fellowship at Arrowhead
When I applied there were about 12 programs in the country that met the Society of Emergency Medicine PAs (SEMPA) Standards for Postgraduate training. I was accepted into, and chose to attend, the Vituity Emergency Medicine PA Fellowship at Arrowhead Medical Center in Colton, California. Arrowhead’s program is one of the longest running PA postgraduate programs in the country. The 14-month program integrates both didactic and clinical emergency medical education while also immersing Fellows in a wide range of rotations including respiratory therapy, ultrasound, pediatrics, surgery, burn, critical care, orthopedics, pre-hospital medicine, OB/GYN, and corrections medicine. I was also drawn to the program because of the way it utilizes PAs in the emergency department (ED), coupled with the wide complexities of patients.
The Arrowhead Fellowship incorporates a variety of experiences supported by more than 200 hours of lectures. Describing one day in the ED only paints a small picture of what I’m expected to see and learn during my time at Arrowhead. Instead, I want to describe the multiple experiences I could have while a PA Fellow, based on which area of the ED I’m assigned. One thing I appreciate about the Arrowhead Fellowship is that I am expected to become proficient in providing care in all areas of the ED, and with levels of patient acuity and complexity from the benign to severely critical. So far, this hasn’t been easy, but it has helped me grow as a provider.
[Society of Emergency Medicine PAs (SEMPA)]
Arrowhead ED is separated by acuity groups into physical sections that we call “Pods.” As patients enter the ED, they are screened by a nurse and receive a Medical Screening Exam by a provider. During this exam, the patient is triaged, and the decision is made to treat and discharge, order labs and medications, or immediately send back to a more critical area of the ED. For those patients who at initial presentation don’t appear critical enough for a bed, but require further workup, their care is transferred to Pod “R” for reassessment. The higher acuity patients are sent back to Pods B, C, or D, pending room availability. The ED also serves as the County of San Bernardino’s highest-level trauma center and has a dedicated trauma/resuscitation bay. The trauma bay normally sees patients from air or ground ambulances; however, occasionally patients are carried in or walk in and meet trauma criteria.
Pod D: Moderate acuity mixed with psych and incarcerated patients
Pod D is designated for moderate acuity patients, including most psych detentions, patients going to jail who have medical complaints and those who are already incarcerated but exceed the capabilities of local correction facilities. This area has just 10 beds, but often has several patients in chairs, and gets 50 to 60 patients per day. As you can imagine, with this volume and patient type, Pod D has a reputation for getting crazy at times. In Pod D I have seen inmates bloody and bruised from jail fights, patients acutely psychotic or combative secondary to drugs, as well as cardiac arrests and critically sick septic patients, all while also taking care of chest and abdominal pain workups. The word crazy may be an understatement. At the end of the fellowship, PA Fellows are expected to “run” Pod D with little to no help. In this Pod I have learned how to manage multiple patients at once, while constantly triaging and prioritizing patients’ needs.
Pods B and C: Working with residents to treat the most critical
Unlike Pod D, Pods B and C are solely run by a senior physician resident. Our hospital is home to a four-year Emergency Medicine Physician residency which allows me to work with physicians as they are training to meet their board requirements. As a PA Fellow, I oversee one side of the Pod, and report to the senior resident. I often get a lot of autonomy, as the senior resident is frequently busy with traumas, working in triage, or dealing with other critical patients. This side of the department is designed for the most critical patients. Here is where we treat septic shock, strokes, unstable surgical candidates (cholecystitis, appendicitis, etc.), and many of the patients that come to the ED critically ill via ambulance. Here I have coded patients, intubated, started central lines, utilized ultrasound for establishing IVs, performed lumbar punctures and paracenteses. In this Pod I have learned how to stabilize critically ill patients while also getting stronger at diagnosing and treating common emergent medical conditions.
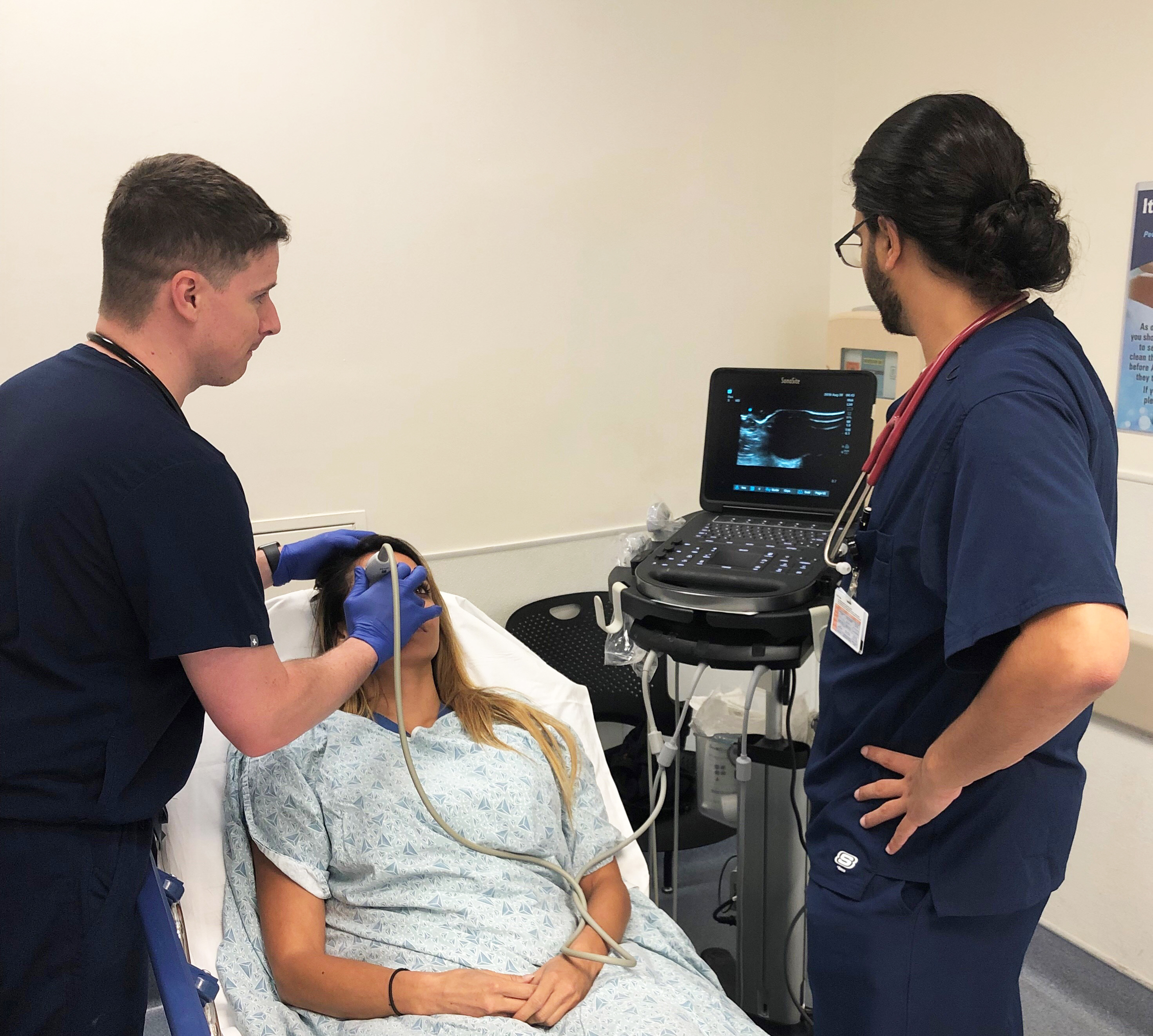
Pod R: Learning the bread and butter of urgent care
Pod R sees patients that are not critical enough for Pods B/C/D but need further workup before they can be discharged. That said, when there are no beds in pods B/C/D, the provider in R could be treating serious conditions such as DKA and sepsis. It’s not unheard-of to close the anion gap of a DKA patient in a Pod R chair while they await a bed in the ICU. Therefore, to call Pod R our “fast-track” would be a gross understatement. Pod R is where I have learned the “bread and butter” of urgent care medicine and where I have developed most of my procedural skills. In this pod I’ve performed countless abscess I&Ds, simple and complex laceration repairs, fracture reductions and splinting, and ultrasound evaluations of the eye, gallbladder, and soft issues. PA Fellows are also expected to “run” this Pod by themselves by the end of their fellowship.
Imposter Syndrome and being ready for anything
Being one of the busiest EDs in California and having only 40 beds, our ED can easily become saturated. When that happens, the designated “high acuity” pods are quickly filled and patients that would have otherwise been moved to these areas are diverted to Pod D or Pod R. Because of this patient movement, I’ve learned that I must be ready for anything. In this type of environment, the Fellowship Faculty has done an amazing job of guiding me through the learning process. They have pushed me to be uncomfortable, but never to the point where I was doing something unsafe. This mentality made this Fellowship extremely difficult, but very rewarding.
One thing that led me to Arrowhead’s program is its association with the University of Lynchburg’s Doctor of Medical Science (DMSc). Since half of the DMSc’s curriculum requires clinical experience, I’ve been able to use my time at Arrowhead towards earning a Doctorate. Seeing the benefit of PAs having doctorate degrees, Arrowhead’s program is paying for my doctorate in exchange for working six extra months at Arrowhead. At the end of my 20 months, I will not only graduate with a certificate from Vituity’s EMPA Fellowship at Arrowhead, but a DMSc degree. The DMSc is an optional path for those in Arrowhead’s program.
To date, the biggest thing I’ve learned from this fellowship is trust in myself. When I started, the burden of Imposter Syndrome (the feeling that I didn’t belong, wasn’t smart enough, etc.) was extremely heavy. In talking to other new PAs, this seems to be a common feeling. I often questioned if I was good enough to be a PA or practice medicine. At times this felt very limiting and caused me a lot of emotional hardship. Gradually I have realized all that I have learned and recognize the impact I am having on people’s lives. While I still struggle with Imposter Syndrome, it is not as omnipresent. This Fellowship has taught me a lot about medicine, but I’ve realized that learning how to balance life with the stress of being a new PA has been much more valuable.
Read More
This PA Telemedicine Director Thinks You Should Explore a Career in Virtual Medicine
A Day in the Life of a PA in a Medical ICU
A Day in the Life of a Critical Care Fellow at URMC
Stephen Lewia is a Director-at-Large on AAPA’s Board of Directors. Contact him at [email protected].
Thank you for reading AAPA’s News Central
You have 2 articles left this month. Create a free account to read more stories, or become a member for more access to exclusive benefits! Already have an account? Log in.



