Boston-Area Health System Shares Lessons Learned from PA Reassignment During COVID-19
PA Crisis Leadership Team Critical During Response
June 15, 2021

The 350 PAs serving across Brigham Health facilities in the Boston, Massachusetts, metropolitan area, retrained under a PA crisis leadership team to deal with the surge in COVID-19 patients in March 2020, and successfully met the needs of patients and the healthcare team.
“Creation of a PA crisis leadership team was paramount to the successful utilization of and support for PAs throughout our COVID-19 patient surge,” says Jessica L. Logsdon, MHS, PA-C, MHA, senior director, PA Services at Brigham and Women’s Hospital (BWH). “We learned important lessons in the process. Having a central resource for PA-related practice is instrumental in being able to rapidly engage the entire workforce in a crisis.”
One of the team members, Lynne O’Mara, MPAS, PA-C, BWH clinical program manager at the Center for Geriatric Surgery, was so moved by the excellent work of the PA crisis leadership team during the COVID-19 patient surge that she is determined to share the story with others.
Creating a team out of nothing
“It’s impressive to take something that didn’t exist and in one week create a whole team structure out of nothing,” says O’Mara, who chronicled the BWH PA crisis team’s journey in a newsletter last summer. “They worked really hard,” she says. “I think other institutions can learn from us and we would like to raise awareness among physicians so that more PAs can do this kind of crisis leadership.”
Prior to the COVID-19 pandemic, BWH’s PA leadership structure had significant silos within departments that lacked an overarching, multi-departmental emergency response element. To better unify PA leaders, Logsdon and Jessica Britnell, MPAS, PA-C, director of emergency medicine (EM), created a PA crisis leadership team. Physicians gave PA leaders the task to make assignments to meet patient needs.
PA leads included Logsdon and Britnell, along with their PA colleagues in other departments: Marissa Cauley, MPAS, PA-C, in inpatient medicine; Jennifer Beatty, MPAS, PA-C, in inpatient surgery; Christie Lucente, MPAS, PA-C, in EM; Michele Elms, MPAS, PA-C, in ambulatory/primary care; Mallory Pingeton, MPAS, PA-C, in ambulatory surgery; and Chelsea Nunez, MPAS, PA-C, and Ariel Nowicki, PA-C, in telemedicine. These PAs were selected based upon their clinical and leadership skills. The crisis leadership team worked together closely to send PAs where they were most needed.
[Wherever you want to go in your career, AAPA can help – join or renew your membership today]
Assessing skills and reassigning PAs
During the initial surge, the PA crisis leadership team leveraged an existing technology platform to centralize information release and training documentation. To ensure PAs were supported during reassignment, the PA crisis leadership team procured in-person training shifts, department-specific documents and videos, and weekly virtual meetings to address individual questions or concerns. Reassigned PAs were also partnered with experienced PAs for at-the-elbow support.
The new PA crisis leadership team assessed the skills, experience, and availability of each PA at the institution, organizing rapid credentialing and training, and developing plans for reassignment. The PA workforce completed a survey to assess years of experience; inpatient responding clinician experience; specific clinical skills related to the management of COVID-19 patients such as ventilator and central venous line management; type of medical record access; and individual reassignment preference.
Combining the survey results and PA work-hour availability, PA leads collaborated with medical doctor (MD) and administrative leaders to create a comprehensive MD and PA surge staffing model. This model was provided to hospital incident command before the patient surge began.
“Thanks to our PAs across Brigham Health, Dana Farber Cancer Institute, and Partners Urgent Care, we were able to collectively persevere through the most challenging of times and emerge even stronger,” says Logsdon. “Our PAs brainstormed, collaborated, and trained together to help stand up new patient care teams in days. They remained strong and steady throughout, risking exposure to themselves and their loved ones to show up for our patients. All of this has been nothing short of miraculous and I have never been prouder to represent such an authentic group of providers.”
“They gathered a group of PAs who were ready to go,” says O’Mara, “which speaks to the fact that advanced practice providers (APPs) can be really important in this type of work. Jess [Logsdon] was the right person since she knows PAs and who can do what. It’s nice to see her experience that kind of leadership. It is also nice to see a group of PA leaders do this work. We all know Jess, she is our director, but seeing eight PAs get together from different sectors – I was really impressed. I wanted people to know about this experience.”
[Treating Patients with Long COVID: A New Frontier for Providers]
Supervising physician restrictions a barrier for PAs
As the surge began, supervising physician restrictions for PAs were a significant barrier. To address this, the Massachusetts Academy of PAs advocated for relaxed restrictions in early March 2020. Massachusetts Commissioner of the Department of Public Health (DPH) Monica Bharel, MD, MPH, quickly signed an order to relax supervising physician and scope of practice guideline requirements for PAs, creating an opportunity for seamless reassignment of PAs across specialty areas.
As a result of the DPH order, central core PA privileges were leveraged to provide a standardized scope of practice for every PA to meet basic patient care needs in any specialty area. To assist with specific procedural skills not covered under basic scope of practice, a team of on-call PAs with procedural experience was created and made available to all reassigned PAs across the institution.
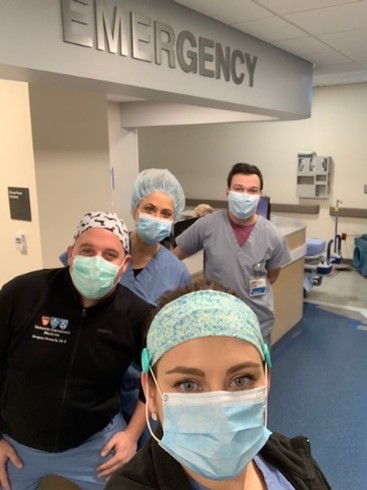
Team environment for reassigned PAs
When COVID-19 patients began arriving in mid-March 2020, the PA crisis leadership team was responsible for managing the staffing of existing medical and surgical units, while simultaneously reassigning staff to areas of need. A master census-dependent schedule was created to ensure appropriate coverage for any sick call or exposures.
Using the surge staffing models, and to support a team environment, PAs were assigned to a demand area and priority matched with attending physicians from their home department. Experienced PAs in critical care and inpatient medicine served as responding clinicians while others with more limited experience provided support for patient rounds and order entry. Emergency and ambulatory medicine, COVID-19 emergency department triage tents, drive-through testing centers, and respiratory clinics were staffed by PAs under the direction of the PA crisis leadership team. The telemedicine PA leaders assisted with quickly integrating virtual visits and virtual rounding programs to address patient needs and preserve personal protective equipment (PPE). PAs were also utilized in miscellaneous roles such as results call-back and as PPE officers, ensuring appropriate technique in PPE donning and doffing for both patient and provider safety.
[PAs Embrace Telemedicine After COVID-19 Jumpstart]
Reassignments highlight PA adaptability
Allison Ruhe, PA-C, works in reproductive endocrinology/infertility in the department of obstetrics and gynecology. When the pandemic hit, Ruhe volunteered to deploy to the general inpatient medicine/special pathogens units. She also helped staff the COVID-19 testing center for patients.
“Being able to transition from a sub-specialty role to a completely different role so rapidly highlights the incredible adaptability of PAs,” Ruhe explains. “The general inpatient medicine PA team quickly developed a system to onboard reassigned PAs by pairing them with an experienced PA. This team-based model worked well and I never felt unsupported or in over my head even though I had limited experience in this role. One of the unique aspects of the COVID-19 pandemic in particular was that all healthcare providers were unprepared. Our collective uncertainty created some comfort in that we all were trying to figure out how to best care for patients together.”
More than 50 PAs were redeployed to roles in ambulatory testing sites, emergency medicine, inpatient medicine special pathogens units, inpatient medicine COVID ICU, and telemedicine and virtual rounding. Some continue to be redeployed to employee testing, COVID vaccine clinics, and infusion clinics.
“Helping people in their most vulnerable moments is the reason I wanted to practice medicine,” says Ruhe, “so the ability to care for COVID-19 patients has been one of the highlights of my career. I have never felt more of a sense of community than during the height of the pandemic in the spring of 2020; we were all in this together supporting each other.”
[How One Health System Trained APPs for COVID-19 in Just 14 Days]
COVID-19 lessons learned in 2020
There are three main lessons learned from BWH’s COVID-19 experience, according to O’Mara. The first is that health systems benefit from PA crisis leadership. “By entrusting PA organization and reassignment to PA leaders, it allowed incident command and hospital leadership to shift their focus to other institutional needs during the COVID-19 surge. It was also budget neutral allowing for resource consolidation and fiscal conservation.”
O’Mara’s second takeaway is about PAs’ flexibility in changing specialties and using their diverse skillsets during a crisis. “Since PAs are trained broadly and can transition between specialties,” she notes, “they often have expertise that extends well beyond their current practice. By surveying staff and building a skillset database, we could thoughtfully reassign PAs based on experience and offer personalized training to those who needed it most.”
The third lesson relates to establishing a leadership structure, especially during a crisis. O’Mara says, “Having dedicated PA leadership to centralize communication and support PA mental health is critical in times of crisis. Sharing information with our PAs used to be difficult; emails and updates came from a variety of organizational locations and departments. We organized communication so PAs could go to a single place to find critical information or voice concerns directly to PA leaders who could work to resolve issues or inform incident command. Finally, the stress of reassignment on our PA workforce was tangible during our crisis response. Having a dedicated PA crisis leadership team who could conduct well-being checks and direct PAs to available support was important to minimizing the negative impacts on PA mental health.”
O’Mara said the team’s conclusions include, “The COVID-19 pandemic highlighted the various ways PAs can be leveraged to complement hospital leadership while maintaining cost and attending to clinician mental health. Although used for a crisis response, the benefits of a PA crisis leadership team extend beyond times of crisis and we are currently exploring ways to continue this structure moving forward. Even though our institution’s APP community is largely comprised of PAs, our PA crisis leadership structure can be broadly applied to APP groups of all sizes and compositions. It has initiated important conversations regarding the benefits of collaboration across APP groups. The future of the COVID-19 pandemic remains uncertain, but the success of this PA crisis leadership structure may provide an opportunity for healthcare systems across the country to consider how to best incorporate PAs efficiently and effectively in times of crisis.”
You May Also Like
PAs Recognized as Vital to Nationwide COVID-19 Vaccine Administration
AAPA Joins Coalition to Advocate for Equitable COVID-19 Vaccine Distribution
PAs Embrace Telemedicine After COVID-19 Jumpstart
Thank you for reading AAPA’s News Central
You have 2 articles left this month. Create a free account to read more stories, or become a member for more access to exclusive benefits! Already have an account? Log in.



