How to Stay on Track in PA School During a Global Pandemic
PA Educator Offers Advice for Applicants and Current Students
July 15, 2020
By Kristopher Maday, MS, PA-C, DFAAPA
COVID-19 has turned everyone’s life upside down and there is not a single person who has not been affected by this pandemic. But the reality is, life must go on. Obviously, safety and health are the primary considerations for everyone across the country, and, as a result, this will make the upcoming months unprecedented in PA education. Future PA students, finishing their CASPA applications and waiting to hear back from their top-choice schools, and accepted students, waiting to start their journey to becoming a PA, will both have new and interesting challenges ahead. Current didactic and clinical students also have potential issues with staying on track for progression and graduation. As a program director, I’ve been thinking a lot about the next few months for PA students and PA programs, and here are my tips for all those involved in PA education.
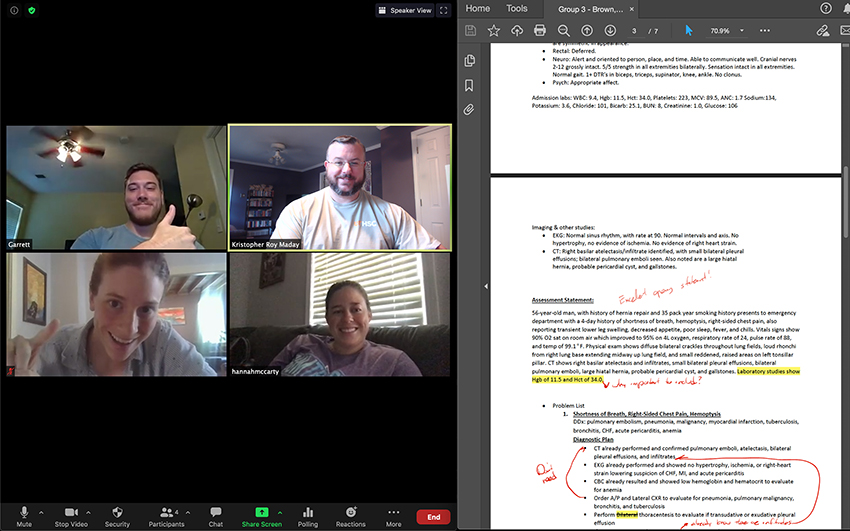
Future PAs in the application phase
- Prepare for virtual interviews.
With the national trepidation around traveling, most schools are planning virtual interviews this summer and fall. There is just too much uncertainty about when it will be safe to congregate in large numbers. Virtual interviews offer both benefits and potential problems. First, this will actually save you a significant amount of money. The cost of interviewing can be upwards of several thousands of dollars if you get selected by multiple schools. The downside is you need to be ready to interview over the computer. Make sure you have a good webcam and reliable internet access on the day of your interview so there are no connection issues. It is hard enough to try to make a connection in a 20-minute interview, but now we have to do it through a screen. You will need to practice! Record yourself talking with family or friends over the computer to ensure you make and keep eye contact, your space is professional (no Zoom virtual backgrounds), and to see how you present remotely.
[Access AAPA’s Student Member Resources]
- Research your schools.
Most programs and universities are already prerecording virtual campus tours. See what your programs are putting together that can help with your decision. Visit websites and social media channels to get an idea of how proactive your program is in thinking about future implications of COVID-19. This will also give you an opportunity to ask direct questions about what programs are doing during the COVID-19 pandemic and how the university is protecting students during their training.
- Decide if this is the right year for you.
This is tough talk, but it’s an important aspect to consider. You have most likely been planning this for the last several years. The last thing you want to think about is whether or not you want to apply this year. Our current PA students have not physically set foot on campus for over three months. They have been responsible for their own time management and staying up to date on assignments and virtual meetings. Some students have managed this well; others have really struggled. Only you can decide if you can handle this type of learning. You also need to think about how you deal with isolation. Part of PA school is bonding as a class and having your classmates to lean on when you are struggling. Whether it is going out after a hard week of exams, working out together, or just having people to commiserate with, you need to think about starting PA school without this camaraderie, and whether that will work for you or not.
[COVID-19 and PA Students: How the Pandemic Affected Me]
Didactic Students
- Get used to online learning.
Imagine having to learn procedures or doing a physical examination online without having the ability to actually perform these skills in front of your faculty. What about learning gross anatomy online? PA students all over the country have been doing this and more and PA programs had to figure out how to offer online learning with almost no time to plan. There will be bumps in the road and things that don’t work. You have to be ready for this and be flexible. Trust me when I tell you that it is just as hard on your faculty. All the frustrations you feel and are experiencing are being felt by your faculty. We recognize that some of the online instruction is not ideal, but understand we are doing our best and have your best interest in mind. We want to give you the best education we can.
- Prepare for interesting schedules.
When it is possible to start bringing students to campus for in-person activities, you may need to be ready to go to class on evenings and weekends. Let’s say that your class has 50 students and your university will only allow 15 students in a physical examination space. This means the program will have to schedule four lab sessions to cover what would have been a single lab. Now imagine this scenario over six other programs on campus with class sizes up to 200 students. Also, you have to factor in 20-30 minutes of cleaning between groups. There is only so much time during a normal eight-hour day. Universities and programs are now exploring scheduling evening and weekend classes to be able to accommodate these in-person activities. You need to be ready for these unusual schedules to keep you on pace to matriculate to the clinical year.
- Get comfortable with being uncomfortable.
One of the biggest concerns my students have now is did they learn enough and will they retain enough as they move through the program. Many programs did not develop their curriculum for this type of format of instruction. Obviously, if it wasn’t designed to be taught online, then there are adjustments that need to be made to meet their learning objectives. Faculty and programs are adapting to this new delivery on the fly and we need our students adapt with us. Grading scales may be changed to pass/fail and there may be more focused feedback from your faculty about your performance in a course. Instead of a traditional multiple-choice examination, you may have an oral examination with your faculty over the computer. Instead of an in-person, simulated patient encounter, you may be remotely asked questions by your faculty on interpretation of physical examination findings, or what questions you would ask your patient. Adapting to this will only increase your clinical resiliency and better prepare you for clinical practice, even if it was not what you were expecting.
[How COVID-19 Changed My PA School]
Clinical Students
- Limit your potential exposures.
Another tough talk item. Social isolation is extremely difficult and even harder during the clinical year. The hours are long, you are always the “new kid on the block,” and making social connections can be difficult. Sometimes all you want to do is go out with your classmates and feel connected. In the COVID-19 era, what you not must realize is anyone could be infected and every interaction you have with another human being result in a positive test. The ramifications of this, during your clinical year, is that you may be pulled from rotations to self-quarantine. If this happens, you run the risk of having to repeat rotations and potentially delay your graduation. As hard as it might be, the less contact you have outside of the clinical arena without proper PPE, the better chance you have to complete your clinical year on time. Make sure you have a support system of family, friends, and classmates with whom you can connect virtually to help you through this phase of your training when you may feel isolated.
- Start planning a delayed graduation date.
The number one priority for PA programs right now is to keep their clinical classes on track to graduate on time. Some programs have already had to make the difficult decision to delay graduation because of missed clinical rotations this spring. Other programs have been able to move core rotations around and get creative with elective rotations during this time to keep their students on pace. What you can do as a clinical student is plan for a worst-case scenario, which is not graduating on time. Start thinking about what you will do financially if you have to complete a rotation after your planned graduation date. Most academic centers are working on waiving tuition and fees for students displaced by COVID-19, but you still need to have a roof over your head and be able to put gas in your car. This is a tough thing to think about, but planning for a worst-case scenario now will help you mentally prepare if it comes to fruition.
- Think about post-graduate residencies.
With the adjustments being made for the clinical year and some programs losing significant clinical time, you need to think about how prepared you are going to be when you graduate. Programs should prepare students for entry-level PA practice and most students are ready for this when they graduate. With the adjustment of clinical rotations and potential decrease in patient exposures, clinical students may not feel quite as prepared to practice as a PA who graduated under more normal circumstances. Also, many healthcare centers, hospitals, and clinics have instituted hiring freezes because the volume of non-emergent and elective patients are significantly down. As a result, PAs and other healthcare providers have been furloughed until volume is back up. In this reality, even if you are lucky enough to graduate on time, there may not be jobs available and waiting for you. Post-graduate residencies could be a good option for new graduates who don’t feel as prepared to start their clinical practice, or are having difficulty finding a PA position. Start looking now at the application process, timeline, and whether or not it may be a good fit for you.
My Personal Plea
All of your faculty are in education for one reason and one reason only: you. We love our students and enjoy nothing more than watching you develop into a competent PA in the short time we are afforded to be in your life. We all know this has been extremely difficult for you as a student, but know that it is just as hard on us. The best parts of teaching are the interactions we have with our students. The conversations about school and life in our offices and the personal connections we make with every single student we have ever taught are what drives us to be the best educators we can. Not being able to see and teach you all in person takes away the parts of this job that help keep us sane and motivated. Losing these interactions have made this transition much harder on us. Please keep this in mind if you get frustrated or mad at us. We are doing our best, just like we know you are doing your best. We will get through this together.
Special thanks to fellow PA educators Adrian Banning, Janelle Bludorn, and Shaun Lynch for helping me put this list together.
Kristopher R. Maday, MS, PA-C, DFAAPA is Associate Professor and Program Director in the PA Program at the University of Tennessee Health Science Center in Memphis, Tennessee. Contact him at [email protected]. Follow him on Twitter @PA_Maday.
You May Also Like
COVID-19 Resource Center
The Ups and Downs of My First Year as a PA
On the Front Lines: PA Student Dustin Norman
Thank you for reading AAPA’s News Central
You have 2 articles left this month. Create a free account to read more stories, or become a member for more access to exclusive benefits! Already have an account? Log in.



