Breaking Ground as Hawaii’s First PA in Rheumatology
October 12, 2017
By Jennifer Walker

After applying to PA school, Christina Starks, PA-C, sat down with Eastern Virginia Medical School’s (EVMS) director of admissions, who encouraged her to apply to medical school instead. But Starks, age 34 at the time, wasn’t interested.
“I really just wanted to practice medicine, and I wanted to get there the fastest way possible,” she says. “I also wanted to be a PA — to have that flexibility to move between specialties. It felt like the right profession for me.”
Months before graduation from EVMS in Norfolk, Virginia, Starks, who has also worked in research and medical and veterinary sales, found out that her husband, who is in the U.S. Navy, would be stationed in Hawaii. There, it is harder for PAs to find work. There are only 300 PAs in the entire state, most of whom practice on the island of Oahu, where Honolulu is located. Starks searched for work for nine months. Then, in 2016, she saw a job listing on Craigslist for a PA at a rheumatology private practice in Honolulu. The job turned out to be a perfect fit. She became the first PA in rheumatology in the state of Hawaii.

Since then, Starks has made an impact on both the profession and her patients. Wanting to change healthcare on a national level, she attended a meeting of the Hawaii Academy of PAs (HAPA) shortly after moving to Hawaii. Soon after, she was voted in as president-elect. Although Starks, who was new to the PA profession, felt terrified and undeserving, the members thought she was qualified because of her diverse background in medicine and experience as a past president of her PA school’s Student AAPA association. She was president-elect from 2015 to 2016 and president from 2016 to 2017.
During that time, HAPA began working to improve some of the supervisory language in the Hawaii State Medical Board’s Administrative Rules that specifies how PAs can practice. Currently, supervising physicians need to “personally review the records of each patient seen by the physician assistant within seven working days,” the language states. This can be an administrative hassle.
“Ideally, the relationship between a physician and a PA should be determined at the individual practice level because each medical setting and practice specialty are unique,” says Starks, adding that HAPA is currently in talks with lawmakers and community physician leaders about the language.
Starks has also worked to build unity among HAPA’s younger generation of PAs by hosting meetings and dinner programs. The State of Hawaii is looking to build a relationship with the University of Washington to start a PA program.
“If the PA association here is strong and gets together, we’ll be able to have a better foundation so when that PA program does come here, it can succeed,” she says.

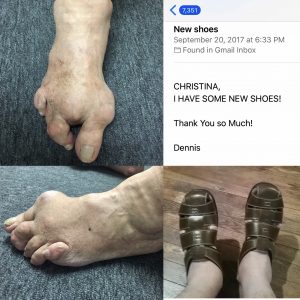
When it comes to her patients, Starks is a committed provider. She remembers treating Dennis Leatherman, a 70-year-old patient with severe gout, a form of arthritis, who lives on the island of Hawaii. The state of Hawaii has 900 fewer physicians than it needs, making access to care a challenge on many of its eight islands. Patients like Mr. Leatherman, who is an illustrator and teacher, often travel by plane to Oahu for care. Because of his gout, Mr. Leatherman had large tophi on his toes and ankles, which are deposits of uric acid crystals that in this case looked like golf balls and softballs. The tophi disabled his joints, making him unable to wear shoes or walk more than 50 feet. He was initially prescribed the traditional form of gout medication.
But Starks, who is passionate about gout because her father suffered from it for more than 20 years, remembered hearing about another novel treatment during CME at the AAPA conference. This biologic treatment for gout is given through IV infusions.
“It’s the only thing that can rapidly reduce the uric acid to help dissolve tophi and possibly change a patient’s life,” she says. So Starks asked her supervising physician if she could change Mr. Leatherman’s treatment plan. He approved the request, as long as she could get coverage for the infusions and flights.
To make the case that this was a treatment Mr. Leatherman needed, Starks talked to his insurance company’s medical director. Her request for coverage was approved. The cost of treatments would be reduced from thousands of dollars to a generic copay, and Mr. Leatherman, who would get an infusion every two weeks, would also have 10 of his flights to Honolulu covered.
The treatments were a huge success. Much of the uric acid from Mr. Leatherman’s joints dissolved, and his tophi shrank. He is now able to walk a mile and a half.
“It changed his life,” Starks says. “I feel blessed to have a skill set that allows me to establish trust and provide medical care to those in need.”
Jennifer Walker is a freelance writer in Baltimore, MD. Contact Jennifer at [email protected].
Thank you for reading AAPA’s News Central
You have 2 articles left this month. Create a free account to read more stories, or become a member for more access to exclusive benefits! Already have an account? Log in.



