On-the-job Stimulation and Work-life Balance Draw PAs to Nephrology
Practicing in Nephrology Gives Solid Foundation in Medicine
December 22, 2021
By Hillel Kuttler
Chronic kidney disease (CKD) presents both a significant challenge for patients and an enormous opportunity for medical professionals in the United States.
More than 37 million American adults, 15 percent of all adults in the country, have CKD, the Centers for Disease Control and Prevention stated in a report it released in March.
Meanwhile, the United States has only 10,000 practicing nephrologists, a situation that is a “supply and demand imbalance,” according to an article jointly published in January by JAAPA and the Journal of the American Association of Nurse Practitioners.
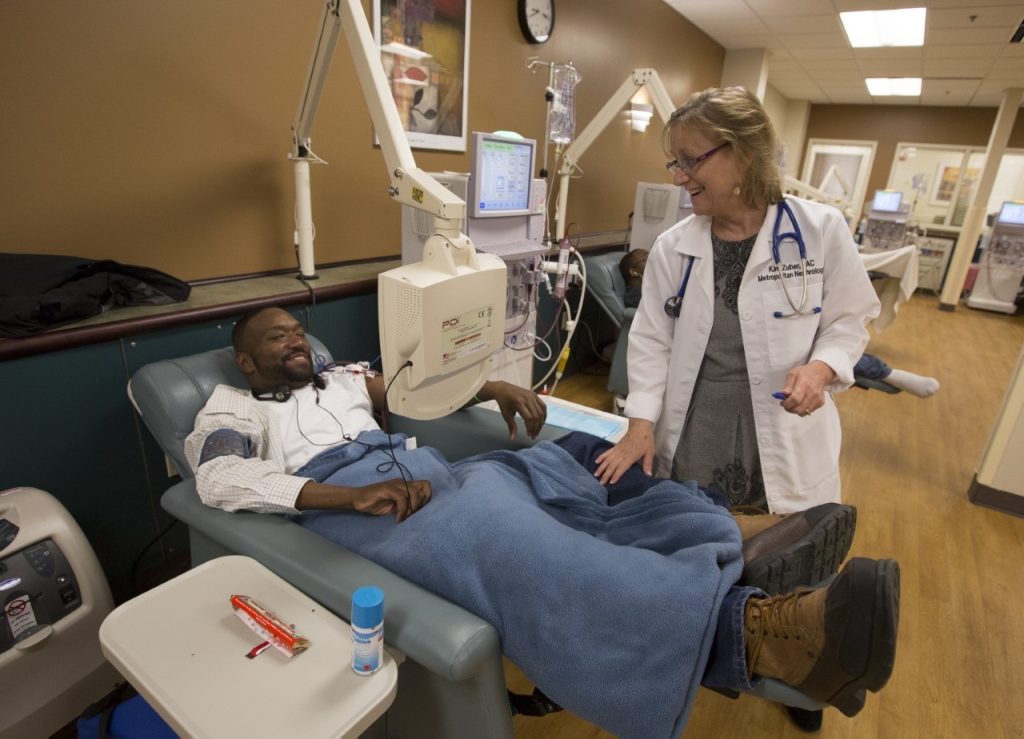
Kim Zuber, executive director of the American Academy of Nephrology PAs, the article’s co-author, and an AAPA Distinguished Fellow, added in a conversation with AAPA that only 350 PAs and 700 NPs work in nephrology.
[Visit AAPA’s CME Central to find CME on nephrology and kidney disease]
Forgotten field of nephrology offers foundation in medicine
Zuber called the specialty a “forgotten field” and says that many young PAs “don’t even know what nephrology is.”
That’s partially because nephrology is seen as a “complicated specialty” that involves multiple conditions and body systems besides the kidneys, she said.
Still, many PAs in other specialties apparently play a role in treating their patients who have CKD. According to preliminary data included in the “2021 PA Practice Survey,” 63 percent of the 1,109 PAs who responded said that they screen, diagnose, treat, or manage patients with CKD.
To Zuber, the challenges of practicing in the specialty – CKD often is accompanied by high blood pressure, diabetes, and cardiovascular disease – also account for nephrology’s attraction, she said.
“If you do nephrology, you can do any internal medicine,” Zuber said. “It gives you such a solid foundation in medicine.”
For those practicing in the specialty, nephrology holds appeal for providing a better work-life balance because it offers more stable schedules than some other specialties. Zuber had worked as a PA in orthopaedic surgery for 15 years but, while pregnant with her first child, shifted to nephrology because, she said, “It is very, very family-friendly.”
Zuber’s refrains were echoed in AAPA’s interviews with three other PAs working in nephrology.
Close bond formed with nephrology patients

Amy Mosman represents the ideal for those looking to address the nephrology-professional shortage. She entered the field immediately upon graduating from St. Louis University’s PA Program and works in her alma mater’s nephrology department.
“I had absolutely zero interest in going into nephrology,” explained Mosman, who’d been interested in general medicine, “yet it ended up being my field. I really just got sucked into it. Now I feel that it’s the only field for me.”
That’s mostly because of the close bonds formed with patients, like one who heads to a casino after completing each week’s dialysis treatments and another who is an artist and draws during dialysis. The latter sometimes drew caricatures of his caregivers; once, a good lab report inspired his next creation.
[Top-notch CME comes with AAPA membership – join or renew today]
Mosman is most gratified when a patient’s dialysis ends because a kidney-transplant donor was found. A downer is when a transplant fails and the patient returns to dialysis.
She said she is stimulated by the diversity of patients’ conditions and by the “pretty nerdy” calculations demanded, like figuring out a patient’s CKD-EPI (epidemiology collaboration) to measure how well the kidneys are filtering.
“You get to dabble in cardiology, pulmonology, critical care, endocrinology. Our patients have lots of comorbidities,” Mosman said. “For me, not having the drone, the same thing over and over, helps me [avoid] burnout. There’s always something a little bit different to spark my interest. Since so many things impact your kidneys, you get to learn about other [systems].”
As a mother to two young children, Mosman appreciates a flexible dialysis schedule that can be adjusted when need be. “If I have to help with my son’s school Christmas party, I work my schedule around it and it’s all good and well,” she said.
As to whether she sees herself remaining in nephrology, Mosman immediately responded, “I do.”
“I’ve really gotten to love everything I can do, and I make an impact,” she said. “I like the autonomy and support I get from my physicians. I love our patient base. There’s nowhere else you can have that kind of relationship.”
Shift to nephrology for better work-life balance

Work wasn’t kind to Erica Davis’s social calendar.
The Washington, D.C., resident is blunt about why she shifted eight years ago from working as a hospitalist PA to nephrology.
“I switched because of quality of life,” she said.
Davis had to work every other weekend for six years, and often worked from 2:00 p.m. to midnight. She missed class reunions and friends’ Saturday-afternoon barbecues.
“It made dating difficult,” she said. “If you tried to plan things with friends and family, you have to give some of that up. It was cutting into my social life.”
Working in suburban Washington for a nephrology practice means lower pay but a more agreeable, 8:30 a.m. to 5:00 p.m. schedule that enables attending events like baseball games of her favorite team, the Washington Nationals. She has most national holidays off and does not take call.
“For me, it was worth it,” Davis said of the change.
She got the job thanks to knowing her current colleagues while working as a hospitalist. Davis wasn’t as passionate about nephrology then compared to now. Mostly, she said, the attraction is “the people” – the patients she’s gotten to know from caring for them weekly on dialysis. It’s their diversity of conditions, too. Some have diabetes and hypertension, along with autoimmune diseases, like lupus and rheumatoid arthritis. Many of her CKD patients have cardio-renal syndrome, with the kidneys suffering due to poor heart function.
The day before speaking with AAPA, Davis got a call from an oncologist of a patient with multiple myeloma. Because the patient is on chemotherapy, his white-blood-cell count was low.
“We’re trying to prevent his getting an infection by giving him prophylactic antibiotics, but it has to be dosed appropriately for his level of kidney function,” she said. “[The physician] asked me what I recommended for the dosing. That happens a lot.”
Educating patients and providing real-life advocacy

Mandy Trolinger brings real-life experience and built-in empathy to her Denver-area job as a PA at Rocky Mountain Kidney Care.
Very real life, as in: having undergone two kidney transplants.
As an undergraduate, she worked summers as a dietetic technician at the same hospital where, as a teenager, she’d undergone the first transplant – from her mother – caused by a type of glomerulonephritis, an autoimmune disease. Post-surgery, Trolinger learned about dietary restrictions to maintain a healthy transplant. That led to her career as a dietician.
While on a dietetic rotation during her master’s-degree studies, Trolinger first learned of the PA profession. By the time her transplanted kidney began failing, Trolinger was working as a renal dietician. Twelve years after her first transplant, she underwent a second transplant, this time from a deceased donor. Three years later, she began studies at Colorado’s Red Rocks Community College PA Program and has worked in nephrology ever since.
Her having undergone the transplants were an example to patients with CKD that “you can still work, enjoy time with family, and live a fairly normal life,” Trolinger said.
Trolinger’s job includes educating patients about their condition and helping with their transition to dialysis and even transplants. That education “is one of the keys” to their long-term success, she explained.
“My selling point,” she said, “is presenting the patient-advocacy side and providing hope for patients.”
Hillel Kuttler is a writer/editor who can be reached at [email protected].
You May Also Like
American Academy of Nephrology PAs
PAs in Nephrology Get Creative with Kidney Health
Thank you for reading AAPA’s News Central
You have 2 articles left this month. Create a free account to read more stories, or become a member for more access to exclusive benefits! Already have an account? Log in.



