D.C. PA Helps Create Better PPE for Airway Procedures
PA Amy Keim Had a Vision Then Made It Happen – In Three Weeks!
November 16, 2020
By Jenni Roberson
When the first wave of COVID-19 hit the Washington, D.C., metro area, Amy Keim, PA-C, an emergency medicine PA, was already working 12-hour shifts at not one, but three hospitals – The George Washington University Hospital (GWUH), Walter Reed National Military Medical Center, and United Medical Center.
“The beginning of the outbreak in D.C. felt like it hit quickly,” Keim said. “Back in early March, PAs were the sole providers in the newly-set-up respiratory complaints section of an ER that was designed to separate possible COVID-19 patients from the rest of the ER population. This ER is in a very low-income, low-resource neighborhood with a significant chronic disease rate. It was incredibly difficult to meet needs of the patients with resources available to us. It was a true challenge to adapt to and integrate the seemingly ever-changing unknowns and variables in the way we practiced emergency medicine.”
Given such a heavy workload, what Keim pursued next might seem like just too much to take on for people in a punch-in-and-out, 9-to-5 job. But as a PA, Keim is always ready to do more for her patients, and COVID-19 only raised the stakes.
[Find COVID-19 Resources here]
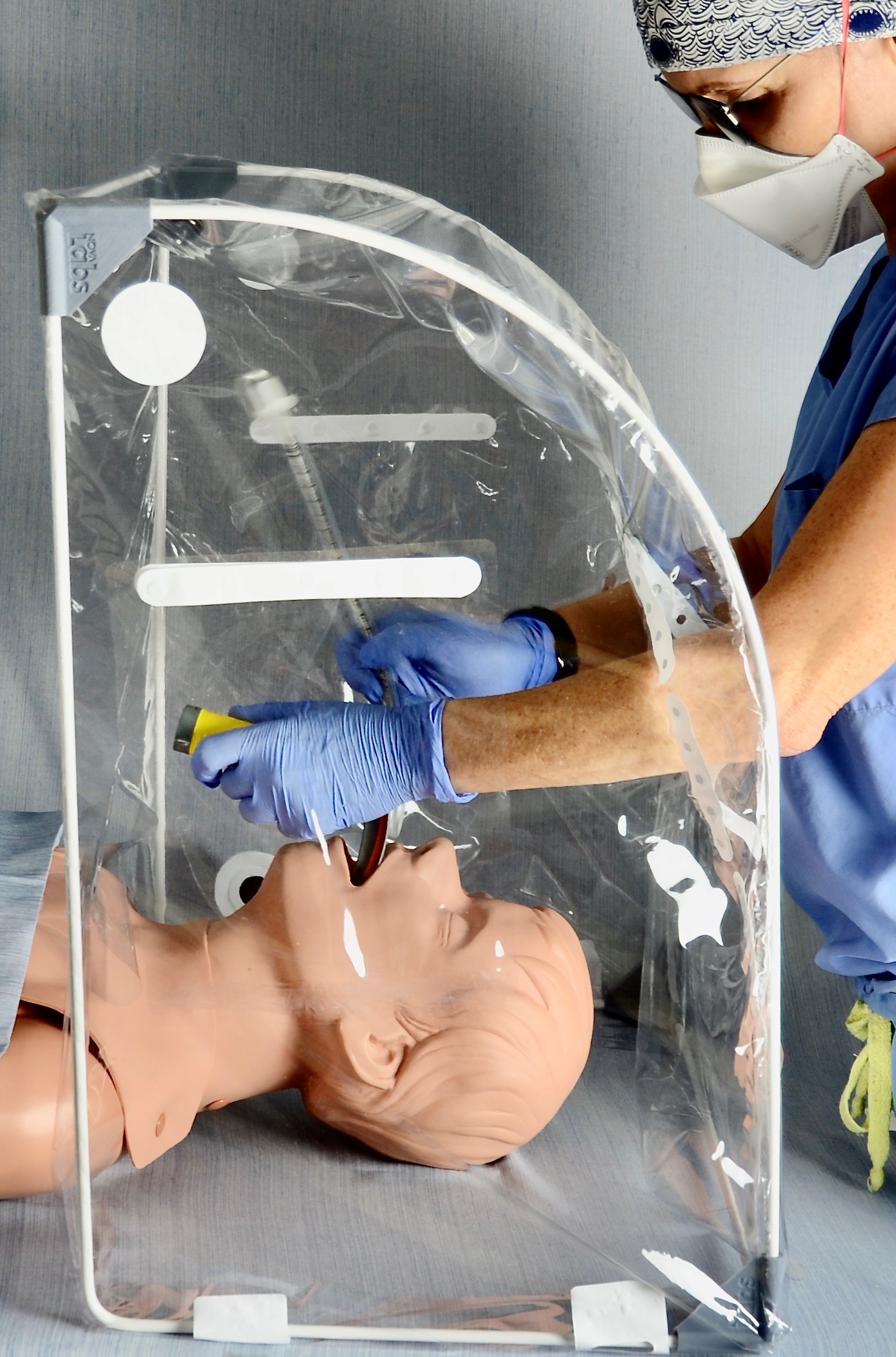
With the sudden influx of respiratory distress patients with suspected or confirmed COVID-19, Keim observed how many hospitals had implemented placing plastic drapes over patients to try to decrease aerosolized particles during airway procedures – PPE that she said she felt was falling short.
“The drapes created significant challenges by interfering with visibility and the mechanics of the procedures themselves while providing an unreliable barrier,” Keim said.
During simulated patient exercises to train medical and nursing staff on practicing new protective protocols, Keim felt compelled to look for a better solution.
“It was while participating in one of these training events, preparing for the inevitable, watching those plastic drapes over the ‘patient’s’ face and the providers struggling against it, when the reality hit hard. How do we balance our safety with that of our patients? There has to be a better way,” Keim said.
From Inspiration to Innovation
Following her aha moment at the training event, Keim did what a lot of people first do when they are looking for answers – she started to Google.
“I went online, and I saw the ‘Intubation Box’ developed by a Taiwanese doctor and adopted in the U.S.,” Keim said. “I saw a lot of problems with using that design in the ER. I thought I had a better solution, so I just started down the path. I had a lot of ideas but knew nothing of engineering or manufacturing. I needed to go from paper to prototype – and fast – so I reached out to a makers group, NOVA Labs, which had a PPE Challenge going. It was pretty amazing. They were organizing volunteers to innovate and make PPE, and they have made some ingenious and important contributions.”
[Learn more about PA member benefits]
Keim said they quickly brought her into their PPE Challenge Slack channel to join forces with her new contacts at NOVA Labs.
“Some truly bright and creative people jumped right into brainstorm the project with me,” she said. “We had the following goals: It had to be easy to make, highly functional, portable, and inexpensive. We wanted it to be made by anyone, virtually anywhere.”
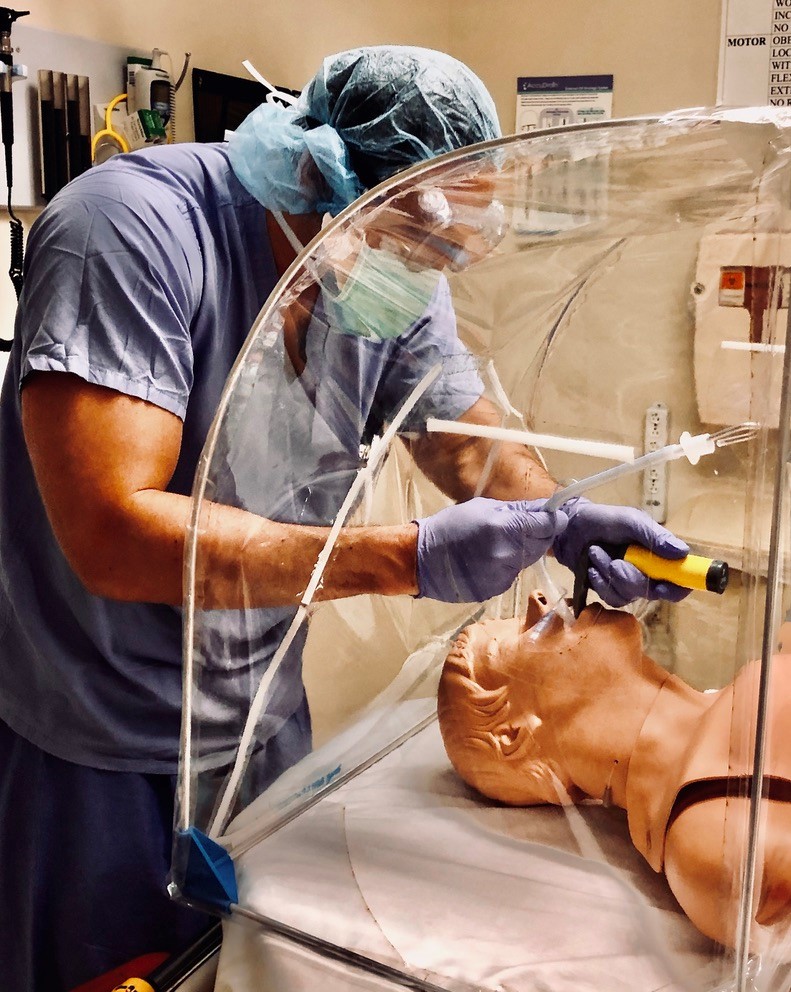
Keim said the project moved fast, and they were testing prototypes on simulated patients within a week. After about two more weeks of designing, building, and re-testing, she said they developed a design for an “airway tent” that they felt would work well.
Getting the Go-Ahead From the FDA
With the prototype complete, Keim’s next step was ensuring they had the ok from the U.S. Food and Drug Administration (FDA) to start rolling it out.
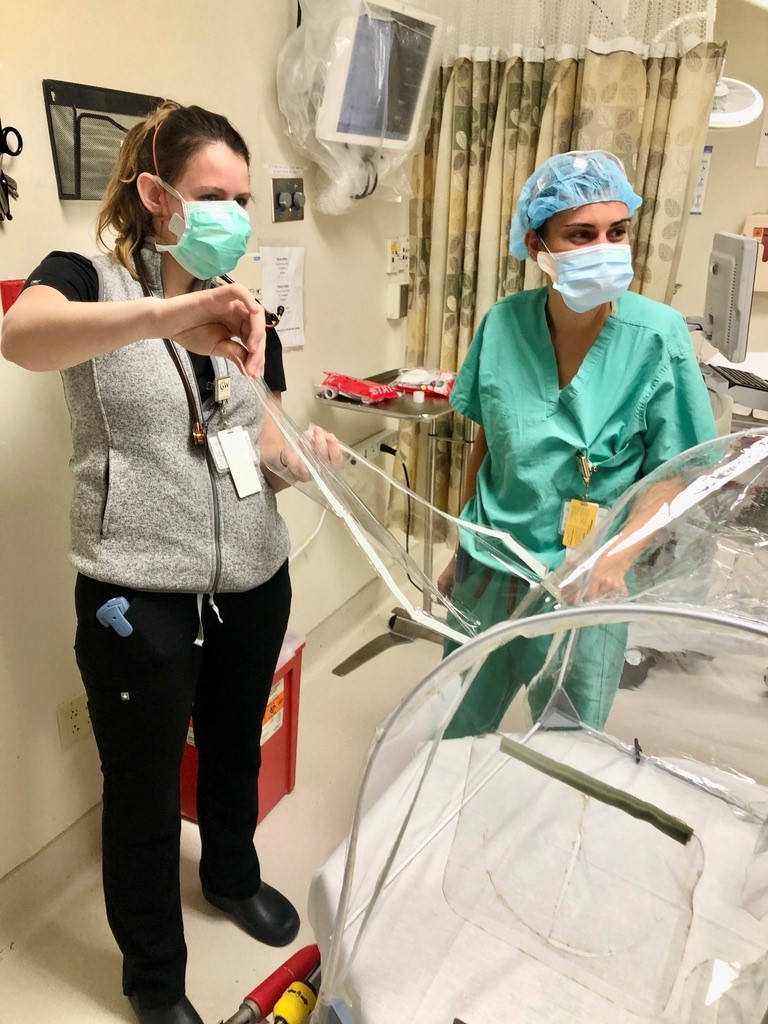
“I reached out to the FDA with the prototype plans, photos and background information to apply for Emergency Use Authorization,” Keim said. “About five days later, I heard back from the FDA that, as a simple isolation device, they did not require authorization for distribution. We immediately deployed tents to the ER, ICU and ORs.”
Fortunately, the speed at which the Airway Procedure Tent (APT) was designed and developed is equally matched with the speed at which it can be reproduced and deployed in hospitals. Without hindrances like patent protections or high shipping costs, the intubation tent is readily available for all clinicians – benefits Keim says she hopes will lead to widespread adoption throughout the pandemic.
“Some other regional hospitals are also using them, and I have more requests that we are working on fulfilling,” Keim said. “It’s been word of mouth only so far. Every time a volunteer builds a tent, we give it to a hospital. We have more requests coming in from hospitals in other states and now some international requests as well.”
More Than Clinicians
Keim says her experience during the pandemic and her journey creating the intubation tent has reminded her that her role as a PA is not just as a clinician.
“Time, creativity and expertise are invaluable tools that we, as professionals, are obligated to use to improve the delivery of care, to promote public health and help bring security to our communities,” she said.
“I am humbled by the role of creative and dedicated individuals who have never taken care of a patient yet have been supporting an entire healthcare system with whatever resources and skills they had. I realize now that there is a much broader definition of healthcare provider than those trained to perform those roles.”
Keim welcomes PAs across the country to reach out to her via email with questions about the tent.
Jenni Roberson is director of Media Relations at AAPA. Contact her at [email protected].
Editor’s note: This article originally appeared in August 2020.
You May Also Like
The COVID-19 Chronicles: PA Shares Frontline Account
How COVID-19 Changed My PA School
On the Front Lines: PA Student Dustin Norman
Thank you for reading AAPA’s News Central
You have 2 articles left this month. Create a free account to read more stories, or become a member for more access to exclusive benefits! Already have an account? Log in.



