The Robot Will See You Now
PAs, and Robot, Help Bring Expert Care to Acute Care Patients
By Steven Lane, MA, MPP
When the medical team makes its rounds in the long-term acute care (LTAC) unit at Cornerstone Hospital in Houston, there are the usual team members checking on the patients—physicians, a PA or nurse practitioner (NP), nurses and perhaps a respiratory therapist. And for the past year or so, another “provider” has tagged along—a robot named Bentley. The robot and its human handlers are part of a new model of care, in which PAs and NPs and a robot provide a 24/7 link to highly specialized critical care physicians, who can log in from anywhere in the country and even the world. This setup is the result of a partnership between Cornerstone’s Telemedicine
Intensive Care Unit Program and iDoc Telehealth Solutions.

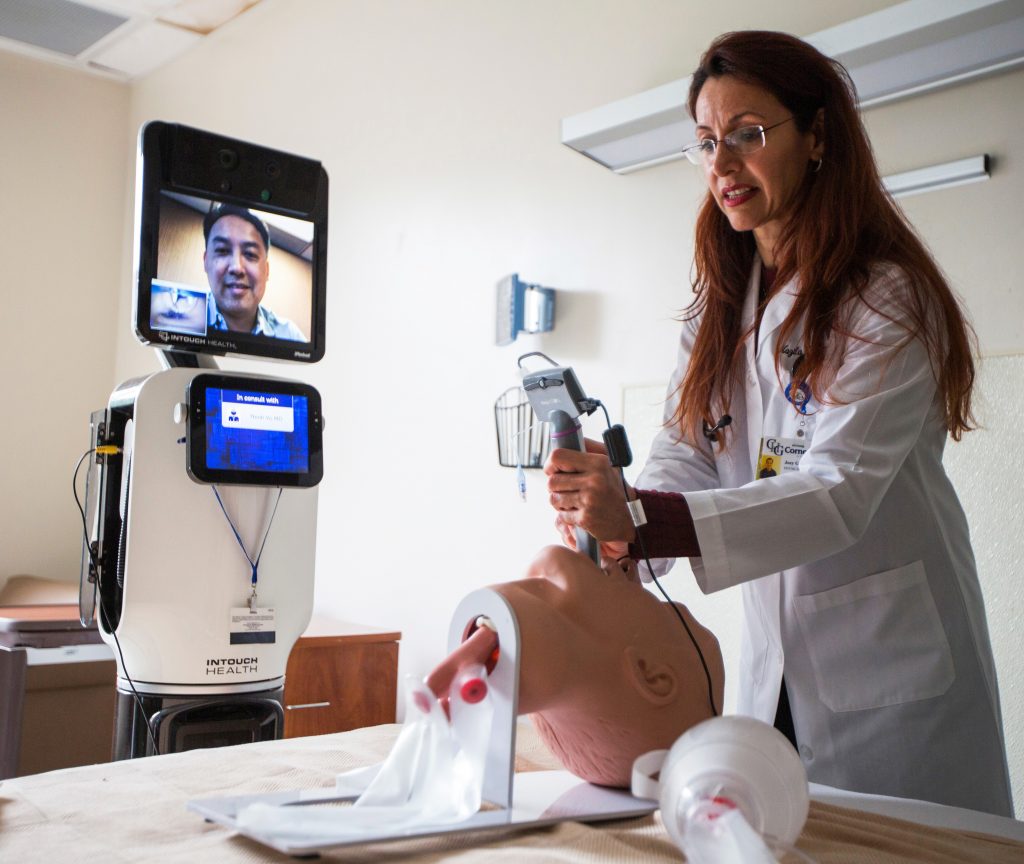
Bentley, the telemedicine robot. Vo can be seen on the screen.
The arrangement is perfectly suited to an LTAC setting, where patients have been released from the ICU but are not yet well enough to go home, says PA Nazila Shagagi, who directs PAs and NPs for the iDoc Telehealth program. Hospitals rarely hire dedicated intensivists to serve as attending physicians for such settings because they cannot justify the expense, given the relatively low acuity level of the patients in an LTAC compared with those in the ICU, Shagagi says.
But this does not mean that there is no need at all for them. So having a board-certified critical care physician on call at a minute’s notice, through the robot, with PAs on hand to manage care the majority of the time, provides the best of both worlds. This model, incorporating the robot and the PAs and NPs into more “traditional” telemedicine, is the brainchild of Imo Aisiku, MD, a neurocritical care specialist who was part of the team that treated former Congresswoman Gabrielle Giffords when she was shot in the head in 2011. Aisiku is now based at Brigham and Women’s Hospital in Boston, but many of his patients are in Houston, at Cornerstone.
A High-Performance Robot
Bentley is named not after Bentley the robot on the children’s show “Fireman Sam” but after the luxury British car brand, a tribute to its high performance engineering and sleek lines. Bentley is a state-of-the-art InTouch RP-Vita model made by the iRobot company. Tall, slender and armless, he looks something like a high-tech water cooler with a screen where his head would be. When Bentley interacts with a patient, the screen projects the face of the remote physician, Aisiku or one of his partners, who can speak to the patient and to the other providers on site.
It is equipped with a very sensitive stethoscope through which the remote physician can hear sounds more clearly than a provider in the ICU, a laryngoscope and very high resolution lenses that allow the physician to do a full neurological exam, including testing for light reaction. A built-in GPS system and a map of the hospital programmed into his software get Bentley quickly to wherever he needs to be and allows the remote physician to be at the patient’s bedside in minutes.
“The main advantage [of having a robot] is we can have the best qualified and most experienced physicians available, wherever they are,” says Shagagi, who came to Cornerstone with Aisiku after working with him for in neuro ICU at another hospital for five years. “We can get the best, most qualified doctor any time day or night.”
Shagagi believes Cornerstone is the first hospital working in this model.
The Role of PAs
Along with Bentley, PAs and their NP colleagues are key components of Aisiku’s model of care. In addition to Shagagi, PA Joey Gee joined the team a year ago, and there are other PAs who fill in occasionally to cover for Gee and Shagagi.
With no full-time attending physicians on site, the PAs have a lot of autonomy, Shagagi says. “I have worked in short-term ICUs for many years, and there is always an attending on site, physically present. This model is different; we have no attending physician except when we call him. That’s why all the staff that we have are quite experienced.”
“Our PAs are an integral part of the team,” says Thinh Vo, MD, one of Aisiku’s partners in the iDoc Telehealth program, who is based in Houston but often uses the robot to evaluate and treat patients remotely after hours. “They function like ICU staff—they evaluate patients on a daily basis; we typically have 8-10 patients on ventilators, very sick people. Without them our quality of care would be far less.”
The quality of care in the ICU has improved markedly since the new model was adopted, both Vo and Aisiku say. “We had some people who really didn’t have the experience with the ICU setting; they were basically moonlighters,” says Vo. “It left a big gap in care. Now, merging telemedicine with robots and our PAs and NPs is something new. The quality of care has skyrocketed, and we have the ability to take care of more complex problems. I am much more confident in the quality of the care we can provide.”
Everybody Loves a Robot
Patients have been very accepting of Bentley so far. “The patients adopt it far sooner than the practitioners,” says Aisiku of the robot. “And what we are recognizing is that medicine is becoming more customer-driven; patient satisfaction is starting to matter more. Patient feedback is extremely positive, and families can dial in as well; we can have bedside discussions and make immediate decisions about end of life.” Bentley helps to improve patient satisfaction by cutting down on wait time and allowing the physician to connect more frequently with the patient and families.
“Through the robot, the physician is able to come in in the middle of the night and can assess the patient immediately; we don’t have to wait for the doctor to come in,” Gee says. “The ability for the doc to instantly address any problem the patient has is unbelievable. Patients are impressed with the technology, and they are impressed they can get to know the doctor.”
Shagagi agrees, noting that patients love Bentley. “Families get amused to see the robot moving around on its own with the whole team following behind. Sometimes kids want to look under the robot to see where the doctor is, or they want to ask the doctor a question.”
The Future of Telemedicine?

Aisiku sees the current project at Cornerstone as the tip of what may be a very large iceberg. “Nationally, this will grow,” he says. “When you think of all the different aspects of our lives that tech has infiltrated, medicine is actually one of the slower fields. We see one-year-olds with iPhones these days. The idea that medicine will not adopt this is just not realistic. It’s just a matter of how.”
The extent to which the role of robots grows in telemedicine will depend to some extent on reimbursement, Aisiku says. At present, Medicare does not reimburse for telemedicine except in very rural areas where it may be the most efficient way to reach a specialist physician. He expects this to change, though. “Healthcare goes the way of Medicare,” Aisiku says. “I envision that Medicare will adopt some form of telemedicine legislation that will expand current coverage.”
“And we are seeing in some states, especially rural ones, the desire for PAs and NPs to have more expansive roles,” Aisiku adds. “In the transition from traditional practice to a fuller use of telemedicine, PAs fit right in. They have the assessment and provider skills in person, but if a PA needs me, I can be there in multiple places. It will be a very complimentary model.”
This article was originally published in the September 2016 issue of PA Professional.
Thank you for reading AAPA’s News Central
You have 2 articles left this month. Create a free account to read more stories, or become a member for more access to exclusive benefits! Already have an account? Log in.




